Congress Proposes ‘PASTEUR Act’ as ‘Superbugs’ Spread and Antibiotic Resistance Increases
Pioneering Antimicrobial Subscriptions to End Upsurging Resistance Act includes subscription-style federal payments and stewardship programs to incentivize development and responsible use of new antibiotics and antifungals.
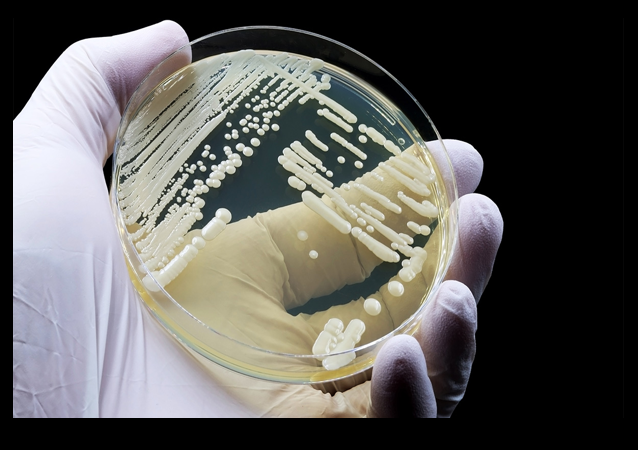
In 2016, I blogged that the Centers for Disease Control and Prevention (CDC) reported the first cases of a drug-resistant and potentially fatal fungal infection had occurred within the United States.
The fungus, Candida auris (C. auris), is known to occur in health care settings such as hospitals and nursing homes. Then, in the spring of 2019, I noted that the CDC warned of the ‘superbug’ fungus sickening hundreds across the country.
As a reminder, C. auris is a fungus that can colonize the skin and can cause severe invasive infections in sick or immunocompromised individuals. In previous reports, I have noted that it has been primarily seen in healthcare facilities, where it spreads easily between patients and via contaminated surfaces. It is also resistant to a range of drugs, making infections challenging to treat.
Ten years later, cases of this fungal infection continue to rise. For example, public health officials are beginning to sound the alarm about infections in New York City caused by both C. auris and bacteria now resistant to antibiotic treatments.
New York has seen a steady increase in Candida auris cases since the state officially detected the dangerous fungus in 2016. Statewide last year, there were 623 clinical cases (those who became sick from Candida auris) and 849 surveillance cases (those who tested positive but weren’t ill).
A study last year determined that the NYC/New Jersey metro area accounts for nearly 20% of the US’s Candida auris cases, with researchers pinpointing high-volume travel and trade with South Asia as the source of the surge.
Candida auris isn’t the only savage superbug waging germ warfare in NYC — medical experts warn that overuse of antibiotics is fueling a rise in “nightmare bacteria” that have developed resistance to most known drugs.
“When somebody has a viral illness, they have a respiratory cold, [an] antibiotic [will] have zero benefit to them, but will have more potential toxicity, both in terms of side effects and reactions, but also in the development of resistance,” Dr. Aaron Glatt, professor and chair of the Department of Medicine at Mount Sinai South Nassau, told The Post.
As if the Clade I Monkeypox weren’t bad enough!
Approximately 7,000 cases of C. auris infections were identified across dozens of U.S. states in 2025.
The review, published in Microbiology and Molecular Biology Reviews, helps explain why the pathogen is so difficult to contain and warns that outdated diagnostics and limited treatments lag behind. It was conducted by Dr. Neeraj Chauhan of the Hackensack Meridian CDI in New Jersey, Dr. Anuradha Chowdhary of the University of Delhi’s Medical Mycology Unit and Dr. Michail Lionakis, chief of the clinical mycology program at the National Institutes of Health.
Their findings stress the need to develop “novel antifungal agents with broad-spectrum activity against human fungal pathogens, to improve diagnostic tests and to develop immune- and vaccine-based adjunct modalities for the treatment of high-risk patients,” the researchers said in a statement.
…Unlike many other fungi, C. auris can survive on human skin and cling to hospital surfaces and medical equipment, allowing it to spread easily in healthcare settings.
“It is resistant to multiple antifungal drugs, and it tends to spread in hospital settings, including on equipment being used on immunocompromised and semi-immunocompromised patients, such as ventilators and catheters,” Dr. Marc Siegel, Fox News senior medical analyst and clinical professor of medicine at NYU Langone, previously told Fox News Digital.
Developments such as these have led members of Congress to propose the Pioneering Antimicrobial Subscriptions to End Upsurging Resistance (PASTEUR) Act, which includes subscription-style federal payments and stewardship programs to incentivize development and responsible use of new antibiotics and antifungals.
PASTEUR would revitalize the antibiotic and antifungal pipeline by changing how the federal government pays for novel antimicrobials — shifting from payment based on how much of a drug is sold to payment based on the value it provides to patients and the health care system.
Under PASTEUR, the federal government could enter into subscription-style contracts with pharmaceutical companies, providing fixed annual payments for access to critically needed antimicrobials, regardless of how often they are used. Payments would be tied to a drug’s impact in three areas: major contributions to patient care, innovation, and benefit to health systems and public health.
…The legislation also strengthens antimicrobial stewardship efforts by establishing a grant program to support antimicrobial stewardship programs in rural, critical access and safety net hospitals and long-term care facilities. Recognizing that a significant share of antibiotic use occurs outside hospitals, PASTEUR also includes a pilot program with funding to support outpatient stewardship.
In light of the relentless spread of Candida auris and other drug‑resistant “nightmare” pathogens, Congress must rein in pharmaceutical lobbyists and ensure that any PASTEUR‑style antimicrobial subscription only rewards demonstrable, rigorously proven clinical breakthroughs.
If lawmakers are serious about public health, they will tie federal dollars to hard evidence that new antimicrobials actually save lives in resistant infections, embed ironclad stewardship and transparency requirements, and demand a meaningful public return for this funding, rather than writing blank checks that socialize risk and privatize profit while hospitals struggle and families suffer.
The “trust the experts” approach is no longer valid.
Image by perplexity.ai
Donations tax deductible
to the full extent allowed by law.








Comments
“subscription-style contracts with pharmaceutical companies, providing fixed annual payments for access to critically needed antimicrobials, regardless of how often they are used.”
Recognize this for what it is: an insurance premium. This will help you more easily imagine all the ways it can be exploited as a crony-capitalist scam by Big Pharma.
Don’t call me ‘anti-vax’,dear. The Name’s Mrs Doubtpfiser…
That’s funny as heck.
We keep medical facilities too clean. We wipe surfaces down with stuff that kills “99.9%” of germs, when it’s the 0.1% they don’t kill that we need to worry about. And we just killed off all their competition.
Patients who’ve undergone extended antibiotics regimens sometimes get superbug infections in the colon, and one effective treatment is a fecal transplant, where stool from a healthy donor is inserted into the patient’s colon to reintroduce the normal bacteria population into the system, ultimately outcompeting the superbug.
Before I had surgery some years back I was told to wash with a special antimicrobial “soap” several days prior. I told the nurse I was not going to do that because it would destroy my own “friendly” bacteria which would fight invasive foreign bacteria. If I used the special soap it would give the the foreign bacteria a open field (so to say). I told her I would take a regular shower with regular soap as well as sleep on clean linens. I told her I was confident the surgical site would be properly cleansed by the surgical team and the OR would be sterile.
That was in 2014. Since then I’ve noticed several medical sites have changed their preoperative instructions to patients to allow the use of regular soap
It starts with over-prescribing children with antibiotics at the first sign of illness, without doing the proper tests to determine if antiobiotics are needed. Many mothers can attest to this.
There is good evidence that when hit with antibiotics, such as those that attack the cell wall, that pathogens can change their morphology to “hide” from antibiotic action. And that later they can shift back, making it appear to be a re-infection which is often worse than the original, plus going from acute to chronic infection.
I’m glad that all the time they’re not wasting on fixing our existential election fraud problems is being wisely spent on constructing incomprehensible titles with “clever” acronyms for makework bills.
Your own skin microbiota may be your best defense.
I admit much of the following article is above my pay grade but I found it very interesting nonetheless.
“Role of Microbiota in the Skin Colonization of Candida Auris”
https://pmc.ncbi.nlm.nih.gov/articles/PMC9942586/