Ebola epidemic linked to new mutation
Deadlier strain became easier to spread.
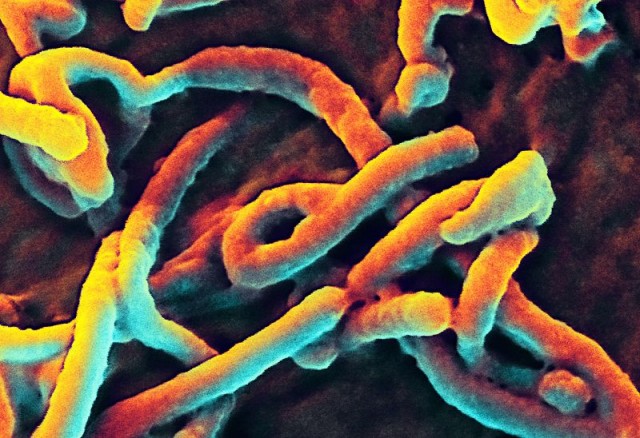
At the beginning of 2016, I noted that the Ebola epidemic that began in 2014, which West Africa hard and resulted in several Americans being stricken by the often deadly virus, had subsided.
Researchers are now reporting that the significant outbreak was the result of a mutation that made the virus easier to transmit and deadlier to human who were infected.
In one study led by 16 researchers at the University of Massachusetts, Broad Institute and elsewhere, genomic analyses pinpointed parts of the Ebola virus that changed during the west African outbreak. One genetic mutation, in particular, appeared to affect a key region of the pathogen where it binds to human cells.
Lab tests confirmed the mutated virus could better infiltrate the cells of humans and other primates. The change was so small that earlier computational analyses of genome differences had not picked it up, says Jeremy Luban, a virologist at the University of Massachusetts Medical School who co-authored the study.
Yet this relatively subtle modification may have had an outsized effect. Gaining easier entry into human cells may have enabled the virus to replicate more quickly in a host—and those greater numbers could make it more likely to jump to the next person, Luban says.
Along with faster transmission rates, the mutation was also associated with higher death tolls. People infected with mutated Ebola virus that dominated the recent epidemic appeared to be twice as likely to die as those infected earlier in the same outbreak with a strain of virus that did not have that specific mutation, the researchers found.
The viral mutation appears to have arisen shortly after the first episode in the 2014 outbreak was reported.
According to Luban, that mutation developed about three months into the outbreak, and went on to dominate the rest of the epidemic. In fact, it was the only version of the virus that spread to other countries and appeared in the infected man who traveled to Texas.
And while the results are not 100 percent, “The whole thing fits together,” he said.
But only Ebola’s individual components were studied. The next step is to conduct more comprehensive experiments in the context of the whole virus, which would require a biosafety level four lab — a status that Boston University’s National Emerging Infectious Diseases Laboratories has been trying to obtain for years. Luban said he has visited NEIDL three times in the past several months to discuss future use of the lab if it does get clearance.
Our reports described how one Dallas nurse, Nina Pham, contracted Ebola while treating a the first patient in this country that came down with Ebola who brought into her hospital. Pham has now reached a settlement with the institution.
Terms of the deal between the hospital’s owner, Texas Health Resources, and nurse Nina Pham, the first person infected with Ebola in the United States, were not disclosed.
Pham sued last year, saying that Texas Health Presbyterian Hospital did not do enough to prevent her from contracting the deadly virus and invaded her privacy after she was diagnosed with it.
The San Diego biotech company that was producing a drug showed promise for Ebola patients has had a less successful result.
ZMapp was perhaps the most sought-after drug at the height of the Ebola crisis, but a clinical trial has failed to prove that patients who got the experimental medication were helped by it.
…After taking a variety of factors into account, the researchers running the clinical trial calculated that there was a 91.2% chance that ZMapp made a difference for patients. That may sound impressive, but it fell short of the 97.5% threshold needed to prove that those who got the drug were more likely to survive than those who didn’t.
Officially, the results of the trial were “inconclusive,” according to a report in Thursday’s edition of the New England Journal of Medicine.
Let’s hope the firm develops a more successful batch soon! Chances are that Ebola will return…and perhaps with a vengence.
 DONATE
DONATE
Donations tax deductible
to the full extent allowed by law.








Comments
A virus tends to continuously mutate and evolve, this makes a long term effective vaccine a rare thing.
What with the mass movement of peoples in various parts of the world in conjunction with the global travel that takes place daily, I would wonder about the potential for medical systems to be overwhelmed to the point of not being able to contain another outbreak, especially if there were multiple ones in various nations.
I wonder if the higher ups at CDC read stuff like this and realize that they need to start an evaluation of their method of handling the next outbreak?
After all, if a virus mutates and evolves, shouldn’t our response to deal with the next crisis evolve with the new information?
With the Muslim invasion of Europe, hopefully none of those monsters get it.
Chances are that Ebola will return.
If the borders aren’t controlled, it will return to the US. And the Democrats—and far too many Republicans—simply won’t control the borders.
So yes, a vote for Hillary is a vote for free ebola for everyone! Even Bernie couldn’t promise more than that.
“Chances are that Ebola will return.”
The reason Ebola is considered a “phantom” virus in Africa is because it appears suddenly then disappears suddenly. When it “disappears”, what its doing is vectoring back into the animal population.
That’s one reason why the Ebola outbreak in the US was so dangerous. If it wasn’t contained, it could vector out into the local coyote population and never really be rooted out.
And, as our government’s response to the outbreak was so incompetent, I wouldn’t be surprised if its found such a reservoir.
The CDC’s response was especially incompetent. I appreciate that they were trying to prevent a panic, but they gave us misleading information when reassured us it was not “airborne”.
The technical definition of “airborne” is determined by the size of the droplets that aerosol. Ebola droplets are too heavy and thus do not meet the standard of “airborne”.
However, when the public was asking if Ebola is “airborne” what they really meant was “If the guy next to me on the bus sneezes and I inhale, can I catch it?” Yes, you can. Even the CDC Director made this point, but much later after many people were put in exposed positions because they trust what the gov spokespeople were spinning.
We were very lucky last Ebola outbreak, like surviving Russian Roulette with 5 rounds in the revolver. It was a clusterfuck. I hope the CDC had good after action reports, instead of the usual corrupt CYA crap we have come to expect from gov bureaucrats. Because next time, Murphy may smile upon us.